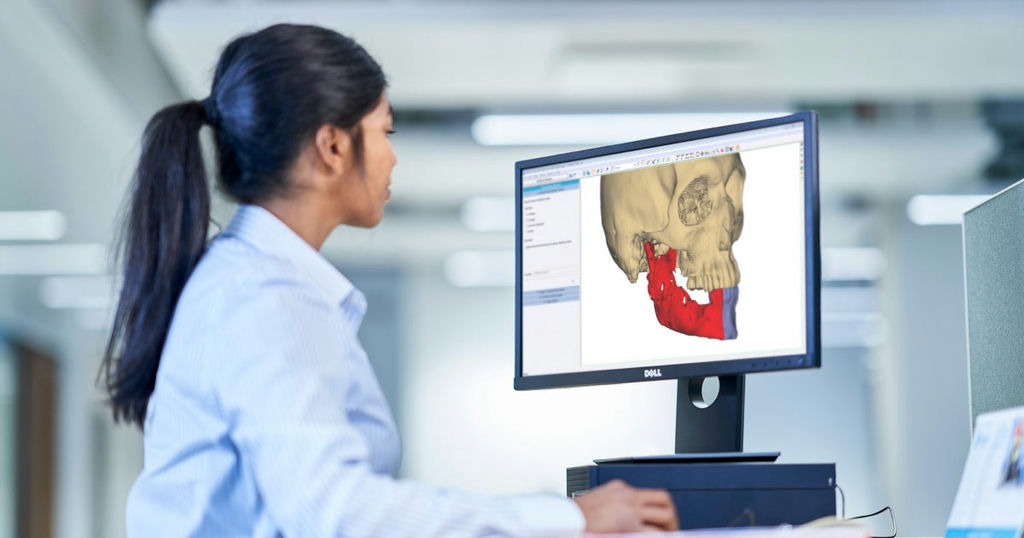
The healthcare sector has embraced 3D planning and printing technologies early on to enhance patient care, with one widely adopted area being in cranio-maxillofacial surgery. For the first part of a special three-part series on 3D Planning and Printing driving personalized healthcare solutions, Chinmay Saraf, Content Editor at AM Chronicle, recently interviewed Dr. Dipesh Rao (MBBS, MDS – Oral Surgery, FIBCSOMS), a distinguished Maxillofacial Surgeon extensively utilising 3D planning and printing technologies.
In this exclusive interview with AM Chronicle, Dr. Rao imparts his perspectives on the incorporation of 3D planning and printing technologies in his practice and delves into the associated challenges and opportunities.

Dr Dipesh Rao is a dually qualified Maxillofacial surgeon and graduated from the Maharashtra University of Health Sciences for Dentistry and the Rajiv Gandhi University of Health Sciences for Medicine. He did his Maxillofacial Surgical training from SDM, Dharwad, which is considered one of the prestigious institutions for this speciality. He was the best outgoing postgraduate student, for which he was awarded the Dr Veerendra Hegde award for academic excellence. Following his Maxillofacial training he completed a one year Cleft lip and Palate fellowship at the Bhagwan Mahaveer Jain Hospital in the year 2010-11.
Globally only a few surgeons have the privilege to have trained in both Paediatric Maxillofacial Surgery and Craniofacial Surgery, and Dr Rao is one of them. He completed his Paediatric Maxillofacial fellowship at the Royal Children’s Hospital, Melbourne, which is considered one of the world’s best Children’s Hospital. He gained his Craniofacial expertise by completing a Royal College of Surgery accredited fellowship at the Oxford Craniofacial Unit. The Oxford unit is globally recognised for its pioneering work in the field of Craniofacial surgery and its well-integrated multidisciplinary practice.
Q1 Could you share your initial experience with 3D planning and printing technology? How did you get started with using these technology in your practice? What were the motivating factors that led you to adopt this technology?
I got introduced to 3D planning and 3D printing while I was in Australia, and they were doing orthognathic surgeries using 3D planning software. So, when I came back to India, I decided that this was something that we would have to incorporate into our practice, and that is how we started doing it with third-party vendors.
Then I realized that if I have 3D planning and printing in-house, it’ll probably be easier to do it at leisure whenever we have time, and that’s how we approached the company to get the , and we started 3D planning and printing in-house.
Q2 How has 3D planning and printing (Surgical guide, personalized implants) transformed how you provide personalized patient care?
Conventional planning is good for two-dimensional planning, but sometimes, in the case of complex movements that deal with all three planes, we require accuracy. With the help of 3D planning software, visualization of complex planes becomes easier, and it also provides a more precise understanding than a CT scan. Hence, overall planning becomes easy, so 3D planning software has become integral to our work.
Q3 Can you share a specific case where pre-surgical 3D planning and printing were used to create a personalized treatment plan or surgical device for your patient? How has 3D planning and printing impacted the outcomes of your surgeries?
I want to discuss the case of one particular child who required distraction. In fact, he required multiple distractions because of the quantum of facial asymmetry, and by using the 3D planning software, we could reasonably and accurately predict the vector and the direction in which the distractor should be placed to achieve the desired outcome. The use of 3D planning and printing tools helped us identify the location where the distractor should be placed to guide the vector towards an accurate position. That was where I think we also noticed that if we continued to distract in the same direction, there would be some hindrances from the occlusal plane. That’s when we opened the bite to prevent any interferences. So, we anticipated the difficulties and predicted the quantum of movement and the direction of movement, all using the3D planning software. The results were appreciable because it was as planned, and subsequently, in the next stage, we also incorporated 3D cutting guides for the distractor, which again made it much easier for us to eliminate any doubts during the surgery. So, I guess this one particular child gave us a lot of insight due to the significant facial asymmetry. It could not have been done as accurately as we planned without 3D planning and 3D printing.
Q4 What are the challenges of using 3D planning and printing for cranial-maxillofacial surgery?
My first challenge is finding adequate time to perform 3D planning and printing process. Adding another personnel, like an engineer, would drastically increase the cost. that’s one of the reasons I have not been able to hire an engineer. Hence, I am the engineer for the unit, and I perform the surgeries, which is time-consuming Moreover,, using 3D planning software I can perform a mock surgery before the actual surgery on the computer using the 3D planning software which gives me information about the good orientation. of course, it comes at the cost of spending more time on virtual surgical planning and initial problems regarding cost, and everything worked there.
The other challenge is the cost, which I suppose can be negated quickly. Additionally, the 3D planning software is an expert tool and requires some time to be exceptionally qualified. I am a surgeon, but I hope a dedicated engineer can master it much faster.
Q5 Can you share your experience or thoughts on implementing an in-house 3D POC (Point of Care) facility that serves multidisciplinary teams? Will a 3D POC facility accelerate the planning process by having a shorter turnaround for printing surgical models or splints (in-house)?
Right now, we are trying to ensure that the other departments also try to incorporate 3D planning and printing into their surgeries, but that is still on hold because we are looking to get a full-time engineer. Once the engineer comes in, the other departments will also start using it. But having said that, only the maxillofacial department is using it for now. In the department, I handle virtual surgical planning and research.
The advantage of having it in-house and making it as a point of care is that it also allows us to show the 3D model and surgical plan to the patient at any given point in time. So, it is a perfect tool for patient education. It also provides opportunities for postgraduate and trainee education. Hence, the POC provides better opportunities when compared with the third-party service. Additionally, sometimes you may need some data for your patient case presentation; because you have the 3D planning software in-house, you can always go back and do it and make the presentation from it.
For the printing of the splints in-house, the turnaround time is less because you don’t have to wait for the shipment/ delivery, you don’t have to send anything to the third-party, so the turnaround time is that much quicker. Sometimes, even if you have an issue and if the splints are not fitting well when you try it on the patient, you can always fix it because of some error that you might have incorporated. You can always do it in-house, so that is the advantage of having the 3D printing at point of care in the same hospital.
Q6 What advice would you give to other cranial-maxillofacial surgeons considering adopting 3D planning and printing technology in their practices?
Well, I often say this: 3D planning and printing are almost a decade old, and we are adopting them quite late. Everybody says 3D planning is the future, but they are very present. We must incorporate this technology into our practices as soon as possible because most patients would benefit from its accuracy and precision. Additionally, it becomes predictable for us to offer treatment outcomes to our patients.
3D planning and printing should be utilized routinely. It cannot be done only in a few cases or in problematic cases; it is for all cases. We must move away from conventional planning because there are so many literature-proven, evidence-based benefits of 3D planning.
Q7 How do you think personalized care empowered by 3D planning and printing technology can be more accessible and affordable for patients?
It’s a great question. This natural progression will happen with time because as time passes, technology becomes cheaper. When mobile phones, laptops, and tablets were introduced, they were only available for a select few, but with time, technology became cheaper, and the novelty reduced. So, I hope a similar thing happens with3D planning and printing technology . Once it is cheaper and more affordable, most healthcare professionals can have 3D planning software in their offices. I hope that general affordability will improve over the next 5 to 10 years, and patients will be able to afford quality care.
Additionally, insurance will also come into the picture. Most of our 3D planning is provided to patients free of cost. This is courtesy of an NGO called Smile Dream, which allows us to do it free of cost, so I guess this is how things will become much more accessible to patients from all socio-economic strata. It is not just about patients being able to afford it,insurance companies or NGOs may be able to provide it for them, so this is something that will happen because once the use case and the effectiveness of 3D planning and printing technology.
I have to put on the record the incredible work done by Smile Dream. In the last 18 years that they’ve been with us, they have definitely helped to adopt newer technology to improve patient care; if they have understood this, it is time for everybody else to understand.
Q8 You are particularly interested in Craniofacial birth deformities. How can 3D technology help patients with Craniofacial birth deformities?
I deal with birth deformities of the cranium, the skull, or the head and the facial region. In these deformities or differences there is a head shape that is not very well acceptable, or the face is asymmetric, or either the upper jaw,/lower jaw is more pronounced, or the upper jaw / lower jaw is recessed. So, various combinations may be seen in the craniofacial region. When somebody does not look symmetrical like how most individuals in the population look, there is a stigma that is associated with clinical anomalies. To mitigate these stigmas, we offer surgery. Sometimes, the surgery may be offered not only for aesthetic reasons but also for functional reasons.
Earlier, we used to base most of our work on our experiences or textbooks. .. However, with3D planning and printing technology , most people can see it happen in real-time. While the surgeon is doing the mock surgery in real-time using the 3D virtual platform, he can probably predict the head shape, face shape, symmetry changes, and dimensions. The surgeon can also measure the values, and see whether it is going to affect the surgery in a positive or negative way. So all the predictions are very well informed., The advantage is that we do these craniofacial anomalies procedures for young children and some of these process do require multiple surgeries. In the past, if one surgery did not go as per plan, it would just increase the number of surgeries that would happen in the future. But, with the 3D planning software the chances of multiple surgeries reduces.
The first step of 3D planning is printing a stereolithographic model, which provides the surgeon hands-on experience of the skull before entering the surgical room. The main advantage of it is that it provides proper guidance before the actual process. So as essential as 3D models, with the virtual plans and cutting guides, things are becoming more precise, and with precision, we may be able to reduce the number of surgeries that we are doing on these children. that’s one of the reasons why I think integrating 3D planning and printing technology into craniofacial anomalies has been such a vital cogwheel in my work.
Q9 As a closing thought, where do you see the future of 3D planning and printing going? How do you think the technology will change the landscape of cranial-maxillofacial surgery in the next 5-10 years?
In the future, one of the features that can be incorporated is haptics. With the help of this, the surgeon can sense the fit, understand the orthognathic movements and simulate the surgery prior in the 3D planning software.
I’m also looking forward to the integration of the virtual reality space. For instance, once you plan the surgery on the 3D planning software, you have a post-operative location of the jaw. In that case, you can simulate it and see if your virtual reality platform can visualize where it is going to end. similar to the 3D planning software navigation. Additionally, by wearing some VR lenses, we should be able to see if we have reached our predicted outcomes. There are a few things that are definitely in the pipeline but haptic and VR technology is what I think would be very exciting and more intuitive. As technology improves, we will have more intuitive 3D planning software which will work swiftly because of an improved algorithm. .Right now, it takes some five to ten steps will may reduced to two or three steps in coming future.
Materialise Mimics Medical has been helping many doctors like Dr Dipesh Rao in improving patient outcomes and advancing patient-centric care with 3D technologies
Materialise Mimics Medical has pioneered many of the leading medical applications of 3D printing, enables researchers, engineers and clinicians to revolutionise innovative patient-specific treatment that helps improve and save lives. Materialise Medical’s open and flexible platform of software and services, Materialise Mimics, forms the foundation of certified Medical 3D printing, in clinical as well as research environments, offering virtual planning software tools, 3D-printed anatomical models, and patient-specific surgical guides and implants. For additional information, please visit: https://www.materialise.com/en/healthcare/hcps/point-of-care-3d-printing
Subscribe to AM Chronicle Newsletter to stay connected: https://bit.ly/3fBZ1mP
Follow us on LinkedIn: https://bit.ly/3IjhrFq
Visit for more interesting content on additive manufacturing: https://amchronicle.com